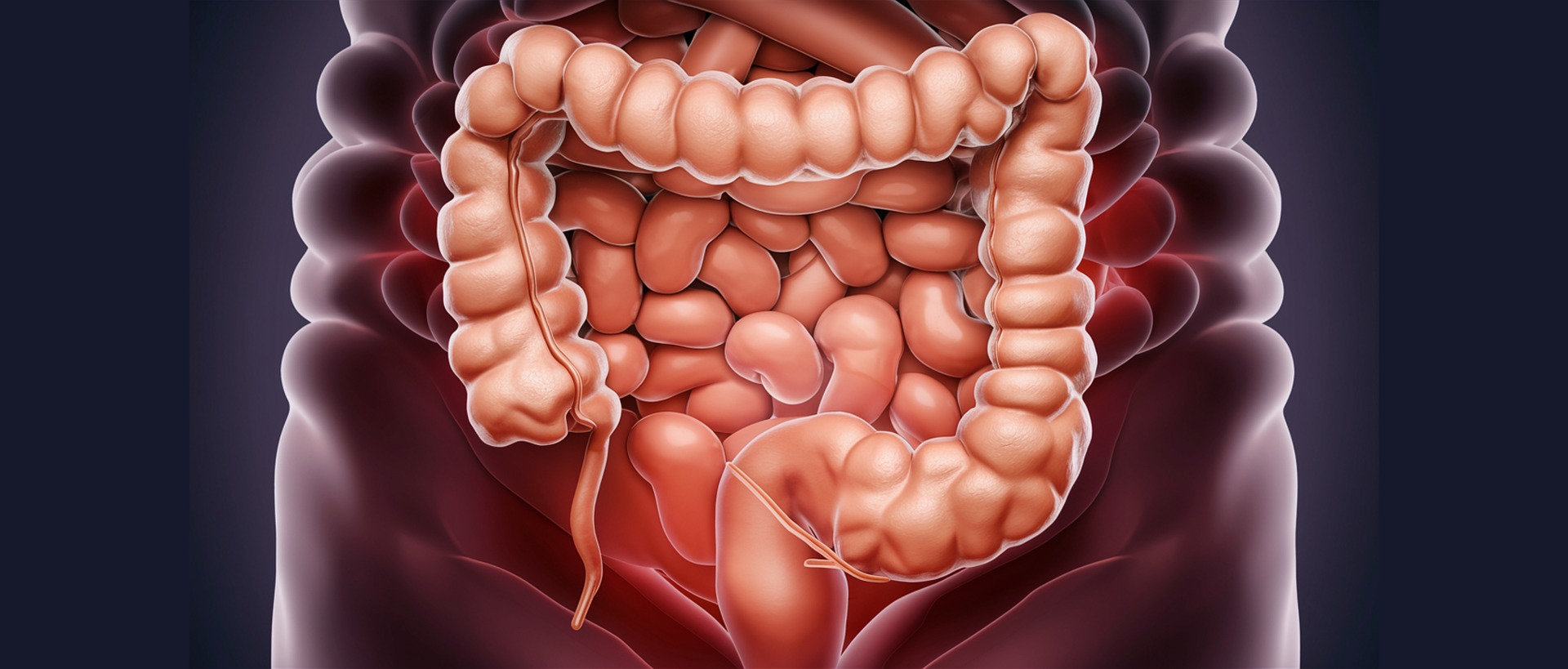
 Crohn’s disease falls under inflammatory bowel disease, which also includes colitis. In Western countries, about 5 out of 100,000 people have Crohn’s. I have had irritable bowel syndrome for over a decade now, so I understand how severe bowel diseases can be. I know a few people who have Crohn’s, and after hearing how debilitating their symptoms are, I felt like my symptoms were just small annoyances. I decided to write this blog to find out if there were any nutritional prescriptions to follow to reduce the symptoms of this disease.
Crohn’s disease falls under inflammatory bowel disease, which also includes colitis. In Western countries, about 5 out of 100,000 people have Crohn’s. I have had irritable bowel syndrome for over a decade now, so I understand how severe bowel diseases can be. I know a few people who have Crohn’s, and after hearing how debilitating their symptoms are, I felt like my symptoms were just small annoyances. I decided to write this blog to find out if there were any nutritional prescriptions to follow to reduce the symptoms of this disease.
What it is like to have Crohn’s Disease
Crohn’s disease cannot be cured, and treatment is aimed at minimizing symptoms and allowing for a higher quality of life. Crohn’s disease is marked by underlying inflammation. Symptoms of this disease are reflective of this inflammatory process and include fever, diarrhea, abdominal pain, weight loss, and rectal bleeding (1). Clinical signs include paleness, weakness, and wasting of the body; perianal fissures (tears in the anal canal that are usually painful, but luckily they are painless in Crohn’s); and anal abscesses (infected cavities filled with pus near the anus or rectum). It can also cause inflammation of the eyes, skin, or joints.
One of the most embarrassing and crippling symptoms is unexpectedly having to use the bathroom and sometimes not making it before having an accident. Every time my friend goes outside the house, she has to make sure she knows where all the bathrooms are in case she has to go. This could present problems at a job that is not sympathetic to people with the disease. Some people have such severe problems that they are unable to maintain a job and instead collect disability. I do not want to spend too much time on the symptoms of the disease, but I wanted to show just how serious, disabling, and painful living with the disease can be.
Under nutrition and malabsorption in Crohn’s Disease
Although Crohn’s can affect any part of the GI tract, the small bowel is involved in 70% of patients, and among these patients, 65-75% of them are reported as undernourished (2). Undernourished means that their diet is not supplying all essential nutrients for the maintenance of proper health. Common reasons for undernourishment among this population include poor dietary intake, malabsorption of nutrients, and loss of part of their intestine. A study involving sixteen patients with Crohn’s disease found that nutrient malabsorption was the greatest contributor to being underweight (2).
Why do Crohn’s patients typically have an inadequate intake of food? Common reasons include anorexia, abdominal pain, nausea, vomiting, and intestinal blockage (2). From personal experience, when my IBS is acting up, I tend to decrease my intake of food since I feel that food may make symptoms worse. It turns out that fear of abdominal pain and diarrhea after eating is the most common reason given by Crohn’s patients for their reduced food intake (3).
Malabsorption was especially high in patients who had ileal resection (removal of part of the intestines). After this procedure, patients had fat, vitamin B12, and trace mineral malabsorption. Those who had a larger section removed had more malabsorption than those who had less of their ileum removed. An interesting finding of this study was that patients who had malabsorption were able to maintain a healthy weight.
It is believed that for the patients with malabsorption, their bodies compensated for decreased caloric intake by lowering the calories used at rest (resting energy expenditure). If calories used to maintain life were lowered to equal the amount of calories ingested, then the patient would be able to maintain weight. Because of this, one observable goal of nutrition intervention would be an increase in their resting energy expenditure, which would indicate that they are absorbing more calories.
A prospective study involving those with Crohn’s disease found that 23% of subjects were malnourished, but even healthy subjects had affected levels of magnesium, selenium, vitamin B12, and ferritin (4).
The link between diet and Crohn’s remission
Most of my blogs recommend a certain diet to help with various diseases. Unfortunately, many studies that have tried to find a link between certain foods and the remission of disease have come up empty. On the other hand, a few studies have found that certain foods make symptoms worse in certain individuals. It appears that which foods make the disease worse varies by person, making it impossible to make general dietary recommendations for everyone who has the disease.
While nutrition may not be proven to reduce symptoms of the disease, proper nutrition can remedy many of the side effects of the disease, such as micronutrient deficiencies and bone loss, and can strengthen the immune system. Even though nutrition cannot cure autoimmune disorders and other diseases, it can still play a huge role in maintaining a proper immune system, which can then reduce some of the health problems and morbidity that diseases cause.
Short term remission using elemental or polymeric formulas
Elemental diets and polymeric diets have been shown to induce remission in Crohn’s. Elemental diets are liquids that contain broken-down nutrients such as amino acids, fats, sugars, vitamins, and minerals. A polymeric diet is similar to an elemental diet but contains whole proteins. While these diets have been proven to induce remission in Crohn’s, they can only be taken for a short amount of time, as one would have to eventually reintroduce solid foods.
Besides not tasting good, elemental diets are usually given through a tube going from the nose into the stomach. I would imagine this would be uncomfortable. A few studies concluded that these diets were as effective as steroids for inducing remission, while other studies concluded that they were not as effective as steroids (5). Either way, they do work, but they are not a practical, long-term solution.
Exclusion diets
One large trial found that some people have food intolerances to different groups of foods (5). The most common food intolerances were for cereals, dairy, and yeast. One study had patients go on elemental diets until they were in remission. Then they introduced one food item a day, and if it caused diarrhea or pain, they would eliminate that food from their diet. They found that patients could maintain remission when excluding troubling foods. While promising, it is extremely difficult to find specific food intolerances, if there are any. In addition, the study found there are various food sensitivities in a larger Crohn’s population, many of which are not related to Crohn’s flare-ups (5). If you would like more instructions for performing food intolerance testing, email me, and I will send you an article.
Total Parenteral Nutrition (TPN)
Another option to induce remission, although expensive and invasive, is total parenteral nutrition. TPN involves delivering liquid nutrients through a vein using a needle or catheter for 10–12 hours per day (6). This can be done at home with the help of a pump. TPN can be used long-term, although there are potential complications and the person would not be able to eat any additional food or calories outside of TPN.
While obviously not suitable for everyone, TPN has produced impressive results for those with Crohn’s. When 30 patients with severe Crohn’s were put on a TPN diet for a few months, 25 out of 30 patients were able to avoid surgery (7). Another trial assigning 51 patients to TPN by mouth, enteral feeding, or partial parenteral nutrition observed clinical remission in 71% of patients on TPN, 58% of patients on enteral nutrition, and 60% of patients on partial enteral nutrition (8).
Enteral nutrition and solid foods
One study assigned 46 Crohn’s patients in remission to an enteral nutrition plus food group or a regular diet group (9). In the enteral nutrition and food group, 60% of the patients were in clinical remission after 12 months. In the regular diet group, 22% of the patients were in remission at 12 months. Enteral nutrition plus solid foods may be a more realistic and healthier long-term solution to reduce inflammation than just enteral nutrition by itself.
Iron deficiency and anemia
Iron deficiency anemia is very common in those with irritable bowel diseases. Possible reasons for this type of anemia include reduced dietary intake of iron, malabsorption, or intestinal bleeding (10). When being screened for anemia, physicians should measure levels of hemoglobin, serum ferritin, and C-reactive protein (10). For those with active disease, these levels should be measured at least every 3 months. People in remission or with mild disease should have their levels checked every 6 to 12 months (10). Since folate and vitamin B12 deficiencies can also cause anemia, those with small bowel disease or resection should get their levels checked at least once a year.
Even if you are not severely anemic, even a slight iron deficiency can have a negative impact on your life by causing a lack of energy, mental fatigue, headaches, and heart palpitations. If iron deficiency anemia is present, the physician will likely prescribe iron supplements. Ideally, intravenous iron supplements will be used since they are better tolerated, more effective, and improve the quality of life more (10). Oral iron may not be able to offset the iron lost during heavy bleeding. Oral iron causes oxidative stress and increases disease activity, and only about 90% of oral iron is actually absorbed (10). If you decide to take oral iron supplements, make sure to avoid delayed-release iron, as it may be released beyond the site of iron absorption and can worsen or cause ulceration at Crohn’s strictures (10).
Iron supplements for anemia
A study involving 46 IBD patients with anemia found that oral iron supplements increased hemoglobin similar to intravenous iron sucrose, but only intravenous iron caused a rise in serum ferritin levels (11). Also important is the fact that 21% of the patients taking oral iron and 5% of the patients taking intravenous iron had to stop the study because of side effects.
A study from Austria talked about using iron sucrose to treat anemia (12). Iron sucrose has been shown to be effective and safe for over 250 Crohn’s patients (12). Finally, a study found that oral ferrous fumarate increased disease activity, caused patients to feel worse, and increased abdominal pain, while intravenous iron had no effect on these parameters (13).
Use of Erythropoiesis–stimulating agents and iron to combat anemia
Erythropoiesis–stimulating agents replace the erythropoietin usually made by your kidneys (14). Erythropoietin causes the bone marrow to produce more red blood cells. Anemia is often marked by decreased production of erythropotein, a hormone produced in the kidneys. They make more red blood cells (which carry oxygen) and raise hemoglobin levels (15). Erythropotein is given as a shot.
Erythropoiesis–stimulating agents have been shown to be effective at correcting anemia caused by chronic disease (Crohn’s disease). To supplement the effects of this treatment, intravenous iron should also be administered. Clinical trials have shown a response rate of 75–100% when using both intravenous iron and erythropoiesis–stimulating agents together (10).
Low folate and Vitamin B12 levels
If serum levels are low for vitamin B12 or folate, supplementation should be started. If you suffer from severe GI blood loss, continuous blood transfusions are not an appropriate therapy for chronic blood loss (10). Options outside of blood transfusions include intravenous iron with or without erythropoietic therapy. Even if a blood transfusion replaces hemoglobin, iron stores still need to be replenished. To assess how well iron replacement therapy is working, those taking oral iron should have their hemoglobin measured within 4 weeks of the start of therapy and even sooner in patients showing symptoms of iron deficiency.
Osteoporosis
A common nutritional complication of Crohn’s is osteopenia (reduced bone mass), with a prevalence of 40–50% and an osteoporosis prevalence of 5–36% (3). Inflammation causes the release of cells that break down bone, compounded by the use of corticosteroids used to treat the disease but also cause the breakdown of bone. On top of that, the absorption of vitamin D and calcium may be diminished.
Protein loss in Crohn’s
Patients with Crohn’s typically have severe protein losses during inflammation. Losses occur through increased breakdown of proteins, loss of protein into the GI tract, reduced liver protein synthesis, and as a side effect of steroid medications (16). Protein-energy malnutrition can cause delayed wound healing, impaired immune response, and impaired skeletal muscle function (17). Hypoalbuminemia (low protein) occurs in anywhere from 25–80% of patients with Crohn’s disease. Reduced dietary intake of protein is also a major factor. Crohn’s often erodes the mucosal layer of the GI tract, which allows protein to leak out (18).
Measuring serum albumin, prealbumin, and transferrin will show if you have low serum protein levels. Because of these factors, a high-protein diet is often prescribed. It would be best to talk to your doctor about it before starting a new diet.
The use of corticosteroids
Studies have found that the use of corticosteroids results in lower bone mineral density. These studies found that only corticosteroid use, not length of disease, disease severity, or previous surgery, predicted lower bone mineral density.
Corticosteroids are very effective at inducing remission in active Crohn’s disease. Unfortunately, these steroids come with a few nutrition-related side effects. Besides thinning bones, corticosteroids can also induce protein loss (19).
Recommended supplements
I could not find any research regarding the effect of liquid supplement drinks like Ensure on flare-ups in Crohn’s disease. I went to a couple forums for people with Crohn’s disease, and they recommended a supplement called Absorb Plus, which was developed by someone with Crohn’s. I have no idea if it works, but I would imagine Ensure and Boost would be similar. I would only drink any of these if you are having a flare-up. They are not meant to replace food for an extended period of time. Talk to your doctor before you decide to take any of these. The website for Absorb Plus is http://www.absorbplus.com/.
If anyone has personal experience with nutritional supplements and whether or not they work for flare-ups, please email me or leave a comment.
Discussion
The most important factor in Crohn’s disease is maintaining remission. This will minimize inflammation and reduce the many side effects caused by inflammation. Iron deficiency anemia, low vitamin B12 and folate, weakening of the bones, and malnutrition or undernutrition are the major issues. This is why it is important to talk with your doctor about taking supplements and having your levels checked at least twice a year. Also, you may be losing protein, so you should consider consuming a higher-protein diet. In addition to having Crohn’s, having vitamin or mineral deficiencies will make you feel worse and cause long-term health problems.
The most effective way to induce remission is through the through the use of steroids and enteral nutrition. Steroids have their own side effects, and enteral nutrition is invasive and inconvenient. While some foods may cause flare-ups, there are no foods consistently found to affect everyone, so eliminating foods is likely not a solution. As mentioned, talk to your physician about consuming some solid foods and using a nutritional supplement like Absorb or Ensure to meet all of your energy and vitamin needs. A supplement may be especially useful if you are undernourished, malnourished, or losing weight.
The bottom line is to try to maintain remission while keeping a healthy weight and avoiding any vitamin or mineral deficiencies. I hope you learned something from this blog. If you have any further questions, feel free to leave a comment or email me.
Sources
- Lichtenstein, G. R., Hanauer, S. B., & Sandborn, W. J. (2009). Management of Crohn’s disease in adults. The American journal of gastroenterology, 104(2), 465-483.
- Vaisman, N., Dotan, I., Halack, A., & Niv, E. (2006). Malabsorption is a major contributor to underweight in Crohn’s disease patients in remission. Nutrition, 22(9), 855-859.
- O’Sullivan, M., & O’Morain, C. (2006). Nutrition in inflammatory bowel disease. Best Practice & Research Clinical Gastroenterology, 20(3), 561-573.
- Valentini, L., Schaper, L., Buning, C., Hengstermann, S., Koernicke, T., Tillinger, W., … & Lochs, H. (2008). Malnutrition and impaired muscle strength in patients with Crohn’s disease and ulcerative colitis in remission. Nutrition, 24(7), 694-702.
- Rajendran, N., & Kumar, D. (2010). Role of diet in the management of inflammatory bowel disease. World journal of gastroenterology: WJG, 16(12), 1442.
- (http://www.nlm.nih.gov/medlineplus/druginfo/meds/a601166.html).
- Müller, J. M., Keller, H. W., Erasmi, H., & Pichlmaier, H. (1983). Total parenteral nutrition as the sole therapy in Crohn’s disease—a prospective study. British Journal of Surgery, 70(1), 40-43.
- Greenberg, G. R., Fleming, C. R., Jeejeebhoy, K. N., Rosenberg, I. H., Sales, D., & Tremaine, W. J. (1988). Controlled trial of bowel rest and nutritional support in the management of Crohn’s disease. Gut, 29(10), 1309-1315.
- Verma, S., Kirkwood, B., Brown, S., & Giaffer, M. H. (2000). Oral nutritional supplementation is effective in the maintenance of remission in Crohn’s disease. Digestive and Liver Disease, 32(9), 769-774.
- Gasche, C., Berstad, A., Befrits, R., Beglinger, C., Dignass, A., Erichsen, K., … & Van Assche, G. (2007). Guidelines on the diagnosis and management of iron deficiency and anemia in inflammatory bowel diseases. Inflammatory bowel diseases, 13(12), 1545-1553.
- Schröder, O., Mickisch, O., Seidler, U., de Weerth, A., Dignass, A. U., Herfarth, H., … & Stein, J. (2005). Intravenous iron sucrose versus oral iron supplementation for the treatment of iron deficiency anemia in patients with inflammatory bowel disease—a randomized, controlled, open-label, multicenter study. The American journal of gastroenterology, 100(11), 2503-2509.
- Kulnigg, S., & Gasche, C. (2006). Systematic review: managing anaemia in Crohn’s disease. Alimentary pharmacology & therapeutics, 24(11‐12), 1507-1523.
- Erichsen, K., Ulvik, R. J., Nysaeter, G., Johansen, J., Ostborg, J., Berstad, A., … & Hausken, T. (2005). Oral ferrous fumarate or intravenous iron sucrose for patients with inflammatory bowel disease. Scandinavian journal of gastroenterology, 40(9), 1058-1065.
- (http://www.webmd.com/a-to-z-guides/erythropoietin-stimulators).
- (http://my.clevelandclinic.org/health/diseases_conditions/hic_Anemia/hic_erythropoietin-stimulating_agents).
- Song, H. K., & Buzby, G. P. (2001). Nutritional support for Crohn’s disease. Surgical Clinics of North America, 81(1), 103-115.
- King, T. S., Woolner, J. T., & Hunter, J. O. (1997). Review article: the dietary management of Crohn’s disease. Alimentary pharmacology & therapeutics, 11(1), 17-31.
- Umar, S. B., & DiBaise, J. K. (2010). Protein-losing enteropathy: case illustrations and clinical review. The American journal of gastroenterology, 105(1), 43-49.
- (http://www.mayoclinic.org/steroids/art-20045692



New topic for me….but very interesting. Keep going with your good job posting things like this! Regards!
Thanks for commenting Bernal! I am happy that you are keeping up with my blogs.
Great blog on Crohn’s…Any chance of a cure and what other medical conditions could be set on by having Crohn’s that you’re aware of…
Hey Imma. Thanks for the kind words. As for a cure, unfortunately there does not seem to be a cure in the immediate future. The disease is so complex and the symptoms vary so much between person that it is hard to find the exact cause of the disease. Unless they find a common genetic link between all people with Crohn’s it will be hard to develop a cure that would work for each person. But science is evolving rapidly so there is always a chance.
The only medical conditions I know of that could be caused by the disease would be anemia or some kind of disease resulting from a vitamin or mineral deficiency or compromised immune system. It may be a different story for those who have had part of their bowel removed. Unfortunately, I was not able to cover this topic, but when I get to it in the future I will let you know.
I had an idea of what Chron;s Disease was but this article made it more clear. I do respect the people that have to live with these symptoms; it does not seem easy.
Recently I had food poisoning (fish), and it was horrible. I know you cannot compare, but it is not fun having stomach problems.